 |
 |
- Search
AbstractObjectivesThe objective of this study was to review our experience in the surgical management of carotid body paragangliomas and evaluate the outcomes and complications according to the Shamblin classification.
MethodsThirteen patients who had been diagnosed and surgically treated for carotid body tumors (CBTs) were enrolled in this study. We reviewed patient demographics, radiographic findings, and surgical outcomes collected from medical records.
ResultsFifteen CBTs were found in 13 patients and 13 tumors were resected. Selective preoperative tumor embolization was performed on six patients. The median blood loss, operation time, and hospital stay for these patients were not significantly reduced compared to those without embolization. The median tumor size was 2.3 cm in Shamblin I and II and 4 cm in Shamblin III. The median intraoperative blood loss was 280 mL and 700 mL, respectively (P<0.05). Internal carotid artery ligation with reconstruction was accomplished on three patients (23%), and they all belonged to Shamblin III (38%). One Shamblin III patient (8%) developed transient cerebral ischemia, and postoperative stroke with death occurred in another Shamblin III patient. Postoperative permanent cranial nerve deficit occurred in three patients (23%) who were all in Shamblin III (P=0.03). There were no recurrences or delayed complications at the median follow up of 29 months.
Carotid body tumors (CBTs) are slow-growing hypervascular tumors arising from paraganglionic cells of the carotid body which acts as a vascular chemoreceptor organ and is usually located in the posteromedial wall of the CCA at the carotid bifurcation. CBTs are most commonly found among paragangliomas that are typically located in four main sites in the head and neck: the carotid bifurcation (CBT), the foramen jugulare (jugular paraganglioma), the middle ear cavity (tympanic paraganglioma), and along the cervical portion of the vagus nerve (vagal paraganglioma) (1).
Surgery is the gold standard for curative treatment of CBTs. The first successful CBT excision was performed by Albert in 1889 (2), and Gordon-Taylor (3) described a safe, subadventitial dissection in 1940. Since the 1980s, devascularization of CBTs by ligation of feeding branches of the external carotid artery (ECA) during operation has been a common practical technique. Recently, van der Bogt et al. (4) proposed a craniocaudal dissection technique that would minimize postoperative morbidity. Although advances in surgical techniques and the introduction of sensitive imaging modalities have significantly reduced mortality, the incidence of perioperative neurovascular complications, especially cranial nerve (CN) deficit and intraoperative hemorrhage, remains considerable (5, 6).
Since Shamblin et al. proposed the classification of CBTs based on the involvement of carotid vessels in 1971, it has been widely used to describe the CBTs (7). Shamblin group I tumors are localized and do not involve the surrounding major vessels, group II are adherent or partially surround the vessels, and group III are large and encase the vessels. The size of tumor is positively correlated with the Shamblin classification because CBTs become more adherent to carotid vessels as they become larger. However, clinical implications of Shamblin classification in perioperative complications or prognosis have not well documented in the literature (8, 9). The purpose of this study was to review our experience in the surgical management of CBTs and evaluate the outcomes and complications according to the Shamblin classification.
We included 15 CBTs of 13 patients who had been diagnosed and surgically treated at a single institute in this study. Patients consisted of 6 men and 7 women, and their age ranged from 34 to 61 yr (median, 44 yr). The medical records of each patient were reviewed for demographic details, radiologic findings, surgical outcomes, and follow up.
Imaging studies included computed tomography (CT) and/or magnetic resonance (MR) imaging for the evaluation of tumor size and Shamblin group. Preoperative conventional angiography was performed in all patients and tumor embolization was accomplished if possible. Preoperative embolization was not routinely performed when the feeding vessels of the tumor are very close to the internal carotid artery (ICA) with a high risk of embolic particle migration to ICA or if there are multiple anastomoses between carotid vessels and tumors, thus complicating identification of the feeding vessels. Tolerance to carotid balloon occlusion was also tested in all patients. Surgery was performed within 48 hr of embolization to avoid recruitment of collateral blood supply and minimize inflammatory reaction in patients who were given preoperative embolization.
The surgical procedures are briefly described as follows: CBTs were exposed through a transverse cervical incision. All neurovascular structures were identified and periadventitial dissections of the carotid artery were performed. Proximal and distal control of the ICA, ECA, and common carotid artery (CCA) were performed before tumor resection. Any feeding vessels supplying the tumor were ligated early, and the ECA was selectively ligated for complete tumor resection. When a portion of the carotid artery had to be resected, vascular surgeons performed carotid artery reconstruction using an autologous saphenous vein or prosthetic vascular graft (Hemashield, Woven Double Velour, Boston Scientific Corp., Wayne, NJ, USA).
The follow up period ranged from 15 to 64 months with a median follow up of 29 months. SPSS ver. 12.0 (SPSS Inc., Chicago, IL, USA) was used for statistical analysis. Differences between the two groups were analyzed by Mann-Whitney test. Significance was defined as a P-value less than 0.05.
Fifteen CBTs were found in 13 patients and 13 tumors were resected. Four tumors (31%) were located in the right and seven (54%) in the left. Two patients (15%) had bilateral CBTs. A multicentric paraganglioma not from the head and neck was discovered in one patient (8%) who had a cardiac paraganglioma. No patient had a family history of paraganglioma. The most common symptom was a pulsatile neck mass without CN deficit. No patient had functioning CBT that presented with palpitations, tachycardia, and hypertension accompanying elevated catecholamine level. Preoperative CN X dysfunction was observed in 1 patient (8%).
CT and MR imaging revealed enhancing mass splaying the ICA and ECA of the carotid bifurcation (Fig. 1), and the median tumor size of 13 CBTs was 3.6 cm (range, 2 to 5.5 cm). One tumor (8%) was Shamblin class I, four (31%) were class II, and eight (61%) were class III. The ascending pharyngeal artery was a major feeding artery for tumors.
Tumor embolization was performed on six patients (46%) with polyvinyl alcohol particles after superselection of feeding arteries. The others were unable to undergo embolization because they had numerous feeding arteries that could reduce the effect of embolization and the potential high risk of cerebral infarction by embolic particles. No patient demonstrated complications following angiography or embolization. Tumor size and Shamblin group was not significantly different between the embolization and non-embolization groups (P>0.05). The median intraoperative blood loss was 400 mL (range, 200 to 1,200 mL) in the embolization group and 550 mL (range, 200 to 1,400 mL) in the non-embolization group. The median operation time was 360 minutes and hospitalization was 8 days for both groups. These parameters of the embolization group were not significantly reduced compared to the non-embolization group (P>0.05) (Table 1).
According to the Shamblin classification, the median tumor size was 2.3 cm (range, 2 to 3.5 cm) in Shamblin I and II and 4 cm (range, 3.2 to 5.5) in Shamblin III (P=0.005). The median intraoperative blood loss was 280 mL (range, 200 to 400 mL) in Shamblin I and II and 700 mL (range, 500 to 1,400 mL) in Shamblin III (P=0.003), and operation time, including ICA reconstruction time, was 240 min (range, 180 to 360 min) and 420 min (range, 220 to 540 min), respectively (P=0.019). Hospitalization was 8 days in both groups (Table 2).
The ECA was ligated in five patients (39%) during operation. After tumor resection, small tears in the ICA in two patients who belonged to Shamblin II and III, respectively, were repaired primarily. A portion of the ICA had to be resected in three patients (23%), and they all belonged to Shamblin III (38%). Of the three cases with ICA resection, saphenous vein interposition was performed on two patients and prosthetic vascular graft interposition on one patient (Table 3).
One patient (8%) had transient cerebral ischemia immediately after operation that was likely associated with manipulation of the ICA during vascular reconstruction. One patient (8%) died of postoperative intracranial hemorrhage after thrombolysis for ICA thrombosis. These complications were all observed in Shamblin III (25%).
Postoperative CN deficits developed in five patients (39%) immediately after surgery, and they all belonged to Shamblin III (63%, P=0.03). They included three CN X, one CN XII, and one superior laryngeal nerve. Two of them who had CN X deficits recovered within 6 months, and postoperative permanent CN deficit occurred in three patients (23%). One patient presented with preoperative CN X dysfunction demonstrated postoperative permanent vocal fold paralysis and eventually underwent medialization laryngoplasty.
Pathologic examination of all tumors revealed benign histology of paragangliomas without cases of malignant CBT. There was no recurrence or delayed complications at the median follow up of 29 months.
Although most CBTs are benign and slow growing, surgical excision is the treatment of choice. Some authors have found that radiotherapy is effective in inhibiting further growth of CBTs. However, it is often considered to be an alternative treatment modality for patients who cannot undergo surgery due to extensive involvement, multiple tumors, and high operative risk (10).
During operation, all neurovascular structures should be identified to reduce complications. Proximal and distal control of the carotid arteries with early ligation of feeding arteries is important to achieve complete tumor resection. Elective ECA ligation can be helpful for tumor mobilization, but the hemostatic effect of proximal ECA ligation is still controversial (1, 11).
When a portion of the ICA must be resected, immediate vascular control and reconstruction are essential. On small tears, primary closure or patch angioplasty can be performed to repair them. In cases of ICA resection, it is necessary to perform interposition graft or ECA transposition. The grafts used for carotid reconstruction include autologous grafts such as saphenous vein and femoral artery/vein, cryopreserved arterial homograft, and prosthetic graft using polytetrafluoroethylene (PTFE) or Dacron. During ICA clamping, carotid shunting can reduce the risk of stroke.
Regarding vascular complications, an incidence of 2% to 13% has been reported for injury of ICA with or without reconstruction (8, 9). The sacrifice of ECA and ICA has been performed as 13-33% and 11%, respectively (9). In our study, ECA ligation was performed on 39% of the patients, and ICA ligation with reconstruction on 23%. It was noted that the incidence of vascular complications was higher than previous literature because our cases included more advanced staged tumor with a relatively small number of total patients.
Cerebrovascular complication such as stroke associated with or without manipulation of major neck vessels can occur, and its incidence has been reported to be 0 to 11% (9, 12). Postsurgical neurological complication such as CN deficit can occur, and the incidence of postoperative permanent CN deficit ranges from 6.9 to 42% (4, 8, 11, 12). The hypoglossal nerve (CN XII) and vagus nerve (CN X) appeared to be most vulnerable to injury from the sacrifice or retraction. In our study, the overall incidence of postoperative permanent neurovascular morbidity was 31%. Permanent CN deficit was found in 23% of the patients, and motality caused by stroke occurred in one patient.
In terms of the relationship between Shamblin group and complication, all patients who had permanent neurovascular morbidity and carotid reconstruction were Shamblin III. These results also support the reports that the Shamblin classification can be used to estimate the postoperative neurovascular complications (6, 11), and early detection and prompt surgical resection of CBTs will decrease surgical morbidity. However, the Shamblin classification has some limitations because it does not reflect how deep tumor infiltrates through the wall of carotid vessels, which decides if it is possible to preserve the carotid vessels. Recently, Luna-Ortiz et al. (9) proposed modification of the Shamblin classification to make Shamblin IIIb which is clinically or histologically confirmed to infiltrate the adventitia regardless of tumor size.
Initial diagnostic imaging studies usually include CT or MR imaging plus angiography. CT shows an avidly enhancing mass at the carotid bifurcation, and MR imaging depicts a mass with the characteristic "salt and pepper" appearance, especially in larger ones (1). Recently, it has been reported that contrast-enhanced MR angiography can be a noninvasive and quick diagnostic tool replacing catheter angiography for the assessment of head and neck paragangliomas (13). The goals of CBT angiography are to provide a vascular road map for surgeons, search for multicentric synchronous tumors, and enable preoperative embolization for prophylactic hemostasis. Additionally, it could evaluate collateral arterial and venous circulation of the brain if an inevitable sacrifice of major vessels were necessary (1).
There has been controversy concerning the usefulness of preoperative embolization. Some authors prefer routine preoperative embolization because it can lower blood flow and decrease tumor size (14, 15). Others have found that selective preoperative embolization can facilitate tumor excision with less blood loss, particularly in larger tumors (Shamblin type II and III) (1, 4, 16, 17), while some groups disagree on preoperative routine embolization due to postembolization morbidity such as the potential risk of stroke by embolic particles (4, 18).
In our study, there was no significant difference in intraoperative blood loss and operation time between the embolization and non-embolization groups. These results suggest that the degree of invasion of tumors to the wall of carotid vessels and surgeon's experience might be more important factors for intraoperative bleeding than the effects of embolization in selected cases. However, it was difficult to draw a conclusion on the effect of preoperative embolization because of the retrospective nature of this study and a relatively small number of patients who had undergone preoperative embolization.
In conclusion, Shamblin III had a high risk of postoperative neurovascular complications. Therefore, early detection and prompt surgical resection of CBTs will decrease surgical morbidity. In addition, a team approach involving head and neck and vascular surgeons and interventional radiologists for the evaluation and management of these lesions will improve treatment outcomes.
References1. Persky MS, Setton A, Niimi Y, Hartman J, Frank D, Berenstein A. Combined endovascular and surgical treatment of head and neck paragangliomas: a team approach. Head Neck. 2002 5;24(5):423-431. PMID: 12001071.
2. Muhm M, Polterauer P, Gstottner W, Temmel A, Richling B, Undt G, et al. Diagnostic and therapeutic approaches to carotid body tumors: review of 24 patients. Arch Surg. 1997 3;132(3):279-284. PMID: 9125028.
4. van der Bogt KE, Vrancken Peeters MP, van Baalen JM, Hamming JF. Resection of carotid body tumors: results of an evolving surgical technique. Ann Surg. 2008 5;247(5):877-884. PMID: 18438127.
5. Hallett JW Jr, Nora JD, Hollier LH, Cherry KJ Jr, Pairolero PC. Trends in neurovascular complications of surgical management for carotid body and cervical paragangliomas: a fifty-yr experience with 153 tumors. J Vasc Surg. 1988 2;7(2):284-291. PMID: 2828696.
6. Westerband A, Hunter GC, Cintora I, Coulthard SW, Hinni ML, Gentile AT, et al. Current trends in the detection and management of carotid body tumors. J Vasc Surg. 1998 7;28(1):84-92. PMID: 9685134.
7. Shamblin WR, ReMine WH, Sheps SG, Harrison EG Jr. Carotid body tumor (chemodectoma): clinicopathologic analysis of ninety cases. Am J Surg. 1971 12;122(6):732-739. PMID: 5127724.
8. Makeieff M, Raingeard I, Alric P, Bonafe A, Guerrier B, Marty-Ane C. Surgical management of carotid body tumors. Ann Surg Oncol. 2008 8;15(8):2180-2186. PMID: 18512105.
9. Luna-Ortiz K, Rascon-Ortiz M, Villavicencio-Valencia V, Herrera-Gomez A. Does Shamblin's classification predict postoperative morbidity in carotid body tumors? A proposal to modify Shamblin's classification. Eur Arch Otorhinolaryngol. 2006 2;263(2):171-175. PMID: 16010570.
10. Carroll W, Stenson K, Stringer S. Malignant carotid body tumor. Head Neck. 2004 3;26(3):301-306. PMID: 14999807.
11. Wang SJ, Wang MB, Barauskas TM, Calcaterra TC. Surgical management of carotid body tumors. Otolaryngol Head Neck Surg. 2000 9;123(3):202-206. PMID: 10964291.
12. Sajid MS, Hamilton G, Baker DM. A multicenter review of carotid body tumour management. Eur J Vasc Endovasc Surg. 2007 8;34(2):127-130. PMID: 17400487.
13. Neves F, Huwart L, Jourdan G, Reizine D, Herman P, Vicaut E, et al. Head and neck paragangliomas: value of contrast-enhanced 3D MR angiography. AJNR Am J Neuroradiol. 2008 5;29(5):883-889. PMID: 18339724.
14. DuBois J, Kelly W, McMenamin P, Macbeth GA. Bilateral carotid body tumors managed with preoperative embolization: a case report and review. J Vasc Surg. 1987 4;5(4):648-650. PMID: 3560359.
15. Schick PM, Hieshima GB, White RA, Fiaschetti FL, Mehringer CM, Grinnell VS, et al. Arterial catheter embolization followed by surgery for large chemodectoma. Surgery. 1980 4;87(4):459-464. PMID: 6245477.
16. Kasper GC, Welling RE, Wladis AR, CaJacob DE, Grisham AD, Tomsick TA, et al. A multidisciplinary approach to carotid paragangliomas. Vasc Endovascular Surg. 2006-2007;DecŌĆōJan;40(6):467-474. PMID: 17202093.
17. LaMuraglia GM, Fabian RL, Brewster DC, Pile-Spellman J, Darling RC, Cambria RP, et al. The current surgical management of carotid body paragangliomas. J Vasc Surg. 1992 6;15(6):1038-1044. PMID: 1597886.
18. Litle VR, Reilly LM, Ramos TK. Preoperative embolization of carotid body tumors: when is it appropriate? Ann Vasc Surg. 1996 9;10(5):464-468. PMID: 8905066.
Fig.┬Ā1A 35-yr-old woman with a characteristic carotid body paraganglioma. (A) Axial contrast-enhanced CT shows an avidly enhancing mass splaying the external carotid artery (ECA) and internal carotid artery (ICA) at the left carotid bifurcation. (B) Axial T1- weighted images show a mass with prominent vascular flow voids. (C) Angiography shows intense tumor blush between the ICA and ECA. 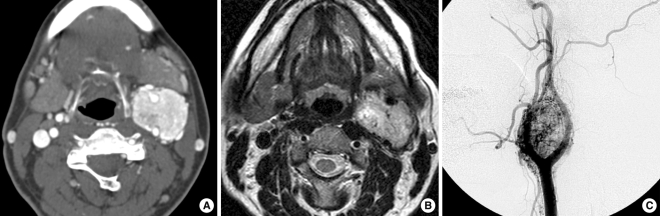
Table┬Ā3Postoperative neurovascular complications according to Shamblin group 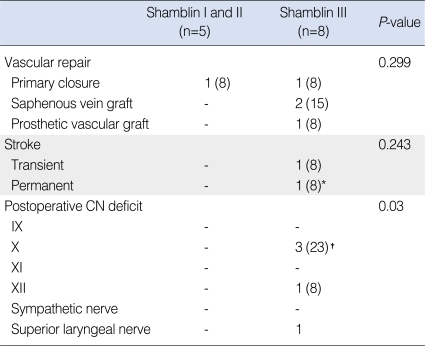 Values are presented as number (%). CN: cranial nerve. *Postoperative intracranial hemorrhage after thrombolysis of internal carotid artery thrombosis caused by postoperative hematoma compression. ŌĆĀVagus nerve paralysis; two patients had transient vocal fold paralysis and one patient had permanent vocal fold paralysis. |
|
||||||||||||||||||||||||||||||||||||||









