|
 |
- Search
AbstractObjectivesDespite sufficient hearing gains, many patients with hearing loss have difficulty using hearing aids due to poor word recognition ability. This study was performed to introduce our hearing rehabilitation therapy (HRT) program for hearing aid users and to evaluate its effect on hearing improvement.
MethodsIn this prospective randomized case-control study, 37 participants with moderate or moderate-severe sensorineural hearing loss who had used bilateral hearing aids for more than 3 months with sufficient functional hearing gain were enrolled in this study. Nineteen participants were randomly assigned to the control group (CG) and 18 patients were assigned to participate in our HRT program once a week for 8 consecutive weeks (hearing rehabilitation therapy group [HRTG]). Their hearing results and questionnaire scores for hearing handicap and hearing aid outcomes were prospectively collected and compared between the two groups.
ResultsAfter completing 8 weeks of the HRT program, the HRTG showed a significantly greater improvement in scores for consonant-only and consonant-vowel sound perception than the CG (P<0.05). In addition, the HRTG showed a significant improvement in hearing ability as measured by two questionnaires (P<0.05), while no differences were observed in the CG. However, word and sentence recognition test results did not show significant differences between the two groups.
ConclusionEven after short-term HRT, patients had subjectively better hearing outcomes and improved phoneme perception ability; this provides scientific evidence regarding a possible positive role for HRT programs in hearing aid users. Further validation in a larger population through a long-term follow-up study is needed.
Hearing loss is a major issue in healthcare. Around 466 million people worldwide were estimated to suffer from hearing loss in 2018, and this number has steeply risen concomitantly with growth in the elderly population [1]. Hearing deteriorates with age, and about 80% of hearing loss patients are elderly [2]. Hearing loss in the elderly causes limitations in daily activity and depression. Moreover, uncorrected hearing loss is related to cognitive impairment, suggesting that appropriate interventions for hearing loss in the elderly are essential [3].
The use of hearing aids (HAs) is a major approach for hearing rehabilitation in the elderly, and its effectiveness for health-related quality of life has been shown in a systematic review [4]. However, the prevalence of HA use in hearing loss patients was reported to be only 17.4% to 37%, and approximately one-third of HAs are not used after fitting [5,6]. The main reason for not using HAs is the lack of significant improvements; this usually involves a scenario where the sounds are louder but the HA user is still unable to understand the words being spoken, especially in noisy environments [7]. This is because HAs can help with the “hearing” process, which simply refers to the perception of sound, but there remains a limitation in listening and comprehension, which is the main process of understanding sound [8]. To overcome this limitation, clinicians need to consider other additional therapeutic modalities for rehabilitation, such as hearing rehabilitation therapy (HRT), for HA users [9].
Worldwide, several web-based hearing rehabilitation programs, such as Listening and Communication Enhancement (LACE) [10] and Customized Learning: Exercises for Aural Rehabilitation [11], have been commercialized. Studies on their clinical effectiveness and usefulness have been proposed; however, the lack of welldesigned prospective studies showing scientific evidence for the effect of HRT makes it difficult to prove that HRT is an effective therapeutic modality.
Moreover, clinical studies on hearing rehabilitation or auditory training in HA users in Korea remain in the early stages. To our knowledge, most reports describing Korean-based auditory training were case reports, and only one case-control study with a small number of enrolled subjects has been published [12]. The aim of this study was to introduce our HRT program and to evaluate its effect on hearing improvement in HA users in a prospective randomized clinical trial.
This prospective study was approved by the Ethics Committee of Seoul St. Mary’s Hospital (No. KC18EESI0403) and followed the tenets of the Declaration of Helsinki. The patient records and information were anonymized and de-identified before analysis. All participants provided written informed consent prior to commencement of the study and voluntarily participated in this clinical trial.
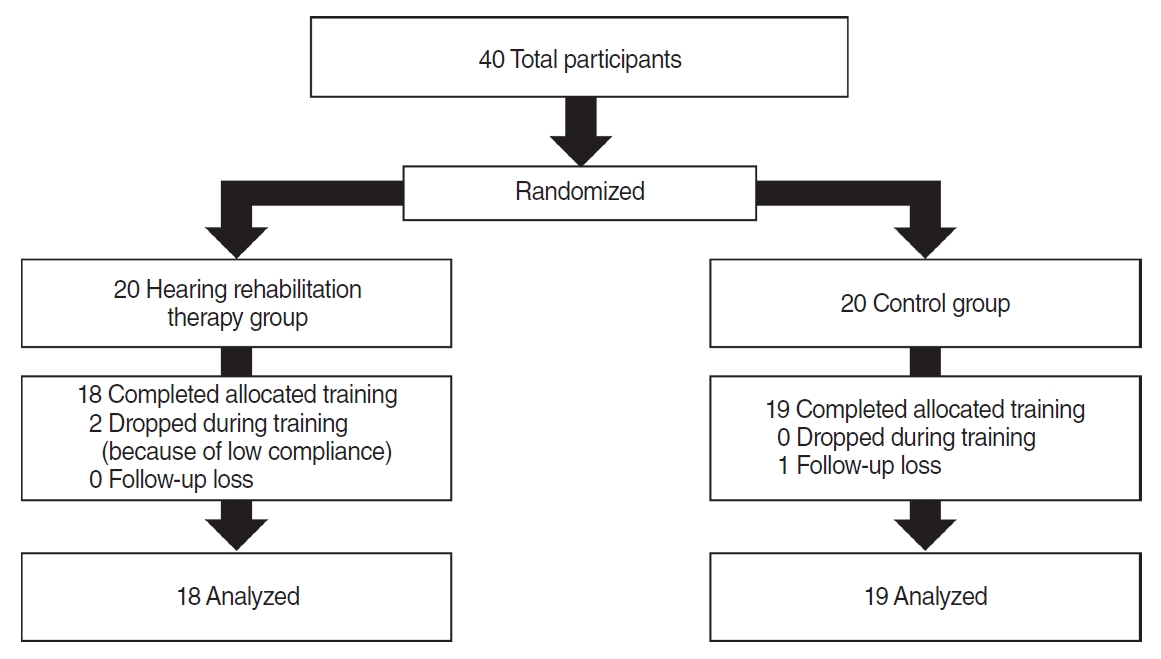
We included 40 participants with sensorineural hearing loss (SNHL) who had been wearing bilateral HAs and were recruited from the department of otorhinolaryngology-head and neck surgery at a tertiary referral center between November 2018 and January 2020. Study eligibility criteria specified adults aged more than 20 years with moderate to severe SNHL in both ears. Moderate to severe hearing loss was diagnosed when the average value of pure tone audiometry (PTA) measured at 500, 1,000, 2,000, and 4,000 Hz was 41 to 80 dB [13]. All patients had used bilateral HAs for more than three months with sufficient hearing gains. They were randomly divided into the hearing rehabilitation therapy group (HRTG) and the control group (CG) by random allocation cards using computer-generated random numbers. Two HRTG participants were excluded at their first visit because of low compliance, and 1 CG participant was dropped during the study period due to follow-up loss (no time to visit). Consequently, the data from 18 HRTG participants and 19 CG participants were prospectively collected (Fig. 1). HRTG participants participated in an 8-week-scheduled HRT program, while CG participants had no interventions. All participants completed assessments including hearing tests and questionnaires on the day of registration and at 4- and 8-week follow-up visits.
Our 8-week HRT program consists of two components: (1) professionals’ face-to-face interview and training sessions: three sessions of doctor’s interview and eight sessions of audiologist’s 30-min face-to-face HRT and (2) daily homework for self-hearing rehabilitation. HRTG participants received our HRT program once a week for 8 consecutive weeks. During the first 4 weeks, consonant discrimination retraining was conducted, followed by retraining in consonant identification and understanding for the next 5 to 8 weeks.
Consonant discrimination retraining consisted of three steps. The first step was to choose whether two sounds with the same consonants were the same or not; for example, if the sounds were M-Ah and M-Eu, the answer is “No.” The second step was similar to the first step but was tested with three sounds with the same consonants. The third step was to listen to three words, two that were the same and one that was different, and to choose the word that was different.
Retraining in consonant identification and understanding was conducted in two steps. The first step was to listen to three words and tell what the other one was, and the second step was to listen to three words and write down what the other one was. All steps were performed under audio-visual conditions and were then carried out under audio-only conditions if the participants had done well in the previous step.
The sound level used in HRT was adjusted to the most comfortable level, and the 10 most frequently used Korean consonants (m, n, r, g, b, h, tɕh, j, s, and s*; from low-frequency to high-frequency consonants) were selected according to Korean National Institute of Special Education-Developmental Assessment of Speech Perception (KNISE-DASP) for training [14]. Low-frequency consonants were used first and retraining gradually moved to high-frequency consonants. If the participant chose more than 85% correct answers during HRT, they moved to the next level.
A self-training handout was provided to the HRTG participants so that they could perform daily HRT at home. The handout consisted of three sessions: first session, words starting with one consonant; second session, words with the same consonant in the middle; and third session, words with a final consonant. Of the 10 consonants selected by KNISE-DASP, low- to high-frequency consonants were used in sequence. The participants were asked to read the words out loud to hear the differences, and a checklist to record the completion of their own training was provided to confirm their compliance of HRT. The average time for self-training as a homework was about 30 to 40 minutes per day, which was similar to face-to-face HRT session in the hospital. The process of the HRT program is described in Fig. 2.
All participants completed hearing tests and questionnaires at the 0-, 4-, and 8-week visits. PTA without HAs and sound field threshold audiometry testing with HAs were conducted to exclude changes in hearing level and inappropriate function of HAs. Audiological outcomes were evaluated with word recognition score (WRS), Korean consonant perception test (KCPT) [15], and Korean speech perception in noise (KSPIN) test [16]. Subjective benefits were measured by two validated questionnaires: the Korean Version of the Hearing Handicap Inventory (KHHIE) and the International Outcome Inventory for Hearing Aids (K-IOI-HA) [17,18].
In order for statistical significance at 0.05 confidence level with 80% power, the sample size required for the two groups was estimated as 18 patients per each group. Allowing for a 10% dropout rate, 42 patients were estimated to be required in total. However, 40 patients finished the study protocol and were finally enrolled in this study, which were the sufficient patient number for statistical analysis.
Statistical analysis was conducted using SAS ver. 9.4 (SAS Institute, Cary, NC, USA). The Shapiro-Wilk test was used to examine the normality of the measured variables. Data was expressed as mean, standard deviation, and percentage. P-values were calculated using the chi-square test or Fisher’s exact test for categorical variables, the Mann-Whitney test or t-test for two independent variables, the Wilcoxon rank sum test or t-test for continuous variables, and linear mixed-effects model for repeated measured variables. Differences were considered significant when the P-value was less than 0.05.
We statistically analyzed data from a total of 38 participants, consisting of 37 participants who had completed the assessment and one CG participant who performed only the first evaluation. The ages ranged from 55 and 86 years, with a mean of 72.7 years, and the male-to-female ratio was 13:25. There was no statistically significant difference in age (P=0.419) or the sex ratio (P=0.428) between the HRTG and CG. All participants used bilateral HAs, which were either completely-in-the-canal (CIC) or receiver-inthe-canal (RIC) (CIC, 63 ears; RIC, 13 ears) types. The mean duration of HA use was 42.2±33.4 months, varying from 3 months to 120 months. No statistically significant differences were observed regarding HA type (P=0.261) or duration of HA use (P=0.392) between the two groups. The better-hearing ear as assessed by PTA average was the right ear in 23 patients and the left ear in 15 patients, and the better-hearing ear did not show a significant between-group difference. The detailed data are shown in Table 1.
In the initial PTA results, there was no significant difference in the average hearing threshold level between the two groups at all frequencies, regardless of unaided/aided conditions or the better/worse ear (P>0.05) (Fig. 3A). The initial WRS also did not differ significantly between the two groups (P>0.05) (Fig. 3B).
Data from one participant who was lost to follow-up after the first visit were excluded from the assessment. There were no significant improvements in the WRS and KSPIN test results in either group (P>0.05). However, the KCPT results showed significant improvement in both conditions (consonants only, consonants plus vowel–a) regardless of HRT (P<0.001) (Table 2). Additionally, the changes in KCPT scores (third visit score minus first visit score) were compared to assess the difference in the degree of improvement between the two groups. The changes in the score for consonants with the vowel “–eu” were 8.83±4.83 in the HRTG and 4.68±4.60 in the CG, and the changes in the score for consonants with the vowel “–a” were 6.39±4.04 in the HRTG and 3.63±3.84 in the CG. Significantly larger mean changes were observed in the HRTG regardless of the test conditions (P<0.05) (Fig. 4).
The K-IOI-HA scores were 25.6±4.5 in the HRTG and 26.1± 4.2 in the CG at the first visit (P=0.701), 28.3±4.2 in the HRTG and 27.3±4.3 in the CG at the second visit (P=0.279), and 29.4± 4.3 in the HRTG and 27±4.5 in the CG at the third visit (P=0.100). In the analysis of the longitudinal data, a significant improvement was observed in the HRTG (P<0.001) but not in the CG (P=0.117).
The K-HHIE scores showed similar results. The initial mean total score was 36.6±28.1 in the HRTG and 33.5±26.3 in the CG (P=0.770), 26.4±26.6 in the HRTG and 29.6±25.8 in the CG at the second visit (P=0.594), and 19.4±20.8 in the HRTG and 28.2±26.4 in the CG at the final visit (P=0.170). There was a significant change between the initial and final visits in the HRTG (P<0.001), but not in the CG (P=0.174). The emotional scores in the HRTG were 17.2±14.8 at the first visit, 12.6±14.1 at the second visit, and 8.2±9.9 at the final visit, while the emotional scores in the CG were 15.7±14.6 at the first visit, 13.6± 14 at the second visit, and 13.3±14.5 at the final visit. The serial mean scores on the social/situational K-HHIE were 19.3±13.9, 13.9±13.4, and 11.2±11.3 in the HRTG and 17.8±12.4, 16.0± 12.3, and 14.9±12.3 in the CG, respectively. Significant improvements in both emotional and social/situational K-HHIE values were observed only in the HRTG (P<0.001 in both scores) based on the analysis of longitudinal data (CG: P=0.228 for emotional scores and P=0.151 for situational scores). These questionnaire results are presented in Fig. 5.
In addition, 12 out of 18 participants (66.67%) in the HRTG and 5 out of 19 participants (26.32%) in the CG showed a decrease of more than 36% in their social/situational K-HHIE scores, indicating significant changes in the K-HHIE scores in both groups [19]. However, the difference in the changes between the two groups was statistically significant (P=0.014).
Compliance is an important factor for better outcomes in HRT, but one study reported that the compliance rate in a cohort of home-based HRT trainees was less than 30% [20]. Other previously conducted randomized controlled trials have reported heterogeneous compliance results. Hickson et al. [21] conducted a controlled study evaluating a group program of active communication education of 2 hours per week for 5 weeks, and only 82 of the 178 participants (46%) completed all the programs. Preminger and Ziegler [22] reported a 91% (31/34) completion rate of 1 hour per week of a group speech perception training program that lasted for 6 weeks, and Humes et al. [23] reported an 87% (13/15) completion rate for a 6-week scheduled at-home auditory training program. Table 3 summarizes the compliance results of other studies [12,21-25].
In our study, only two out of 20 participants in the HRTG had trouble completing our HR program; one was unable to implement the self-home training program due to illiteracy and the other found it difficult to concentrate on the program itself. Eighteen participants who were able to follow our HRT program completed the 8-week schedule, resulting in a high compliance rate (90%).
No consensus has been established regarding the factors or methods that promote better compliance in HRT. However, our 30-minute face-to-face HRT sessions by an audiologist, as well as three separate interviews and reinforcement by an ENT doctor during the 8-week program, seemed to increase patients’ compliance; these components of our program are noteworthy insofar as they differ from the protocols of other studies. It is assumed that reinforcing patients’ motivation by both a trainer (therapist) and a doctor in a face-to-face manner was an important factor contributing to the higher compliance rate during HRT.
The short but intensive method in which our HRT program was conducted, requiring the completion of daily self-home training checklists, might have been another reason for the observation of higher compliance than has been reported for HRT methods involving longer sessions. Shorter training sessions have been proposed to be more effective for auditory perceptual learning as a way to increase compliance [20,26].
The WRS, KCPT, and KSPIN tests were conducted to evaluate audiologic outcomes in our study, but significant improvements were observed only in the KCPT results. There is disagreement regarding whether audiologic outcomes can be enhanced by HRT in HA users. Sweetow and Sabes [24] reported improvements in quick speech in the noise test and Stecker et al. [25] reported improvements in the nonsense syllable test after auditory training. However, other studies reported opposing results, and a meta-analysis concluded that there were no significant audiologic improvements after auditory training [9].
In this study, possible reasons why we did not observe significant improvements in the WRS and KSPIN test results are that our 8-week HRT period may have been too short to show significant results or that our program did not include hearing training in a noisy environment. Further studies with a longer training period and a training protocol including hearing training in a noisy environment will be required to support these hypotheses. In addition, the KCPT scores in the CG also improved at 4 and 8 weeks of follow-up, even though the magnitude of improvement was smaller than in the HRTG. Repeated exposure to the same test or the hearing rehabilitation effects caused by everyday HA use in CG might explain why we observed improvements in KCPT scores in both groups.
As the final goal of HRT in HA users is to improve communication skills in everyday life, self-reported measures might be more appropriate than laboratory speech recognition tests [27]. The HHIE is widely used as a self-assessment tool to quantify the effect of hearing loss on the emotional and situational adjustment of the elderly, and it has been shown to have high reliability and validity [18]. Our study results showed a significant improvement in K-HHIE scores only in the HRTG, in which a higher percentage of participants had significant improvements. The HHIE consists of two subsections; the social/situational subsection contains questions about social disruption due to hearing loss, while the emotional subsection is composed of questions to determine the emotional response to hearing impairment. Our findings showed significant decreases in the scores of both subsections after HRT. Although there are some differences in the intervention methods, previous studies using HHIE as a parameter reported improvements, and our study results support this. de Miranda et al. [28] reported significant decreases in HHIE scores following formal auditory training of elderly HA users, and Lundberg et al. [29] reported improvements in HHIE scores and a depression scale after an educational program with telephone consultations.
The IOI-HA questionnaire has been developed to quantify the satisfaction of HA users and consists of a total of seven questions on daily use, benefit, residual activity, satisfaction, residual participation restrictions, impact on others, and quality of life [30]. In other previous studies, no significant improvement in IOI-HA scores was observed after HA use [29], and it has been suggested that the IOI-HA is not sensitive enough to detect the benefits of HAs [31]. Humes et al. [23] reported no significant improvements in three questionnaires (Profile of Hearing Aid Performance, Hearing Aid Satisfaction Survey, and HHIE) after an at-home auditory training program for HA users.
However, our study and previous studies have reported that HRT or auditory training programs improved subjective satisfaction with HAs, which might be related to the different methods applied. Humes et al. [23] used a computer-based training process, while studies reporting improvements in subjective satisfaction were based on either face-to-face or telephone training [28,29]. The results of various studies are summarized in Table 3.
It can be assumed that hearing training with personal communication rather than a solely computer-based process can be more effective for HA users. The good compliance and therapeutic effect of our HRT program, as evidenced by a prospective randomized case-control study, reveals the value of HRT programs for HA users. The limitations of this study are the relatively short duration of our 8-week HRT program and the small number of participants in this subject-control experiment, which might have been insufficient to show significant improvements in the WRS and KSPIN tests.
This prospective randomized controlled study was conducted to evaluate the effectiveness of our HRT program consisting of specialists’ face-to-face instruction with 30-minute HRT sessions and daily self-administered HRT for HA users. Our HRT program yielded significant improvements in the consonant perception test and self-reporting measures (K-HHIE and K-IOI-HA) and a higher compliance rate than other programs. This HRT program strategy could prove beneficial to many HA users.
▪ The effects of a hearing rehabilitation therapy (HRT) program for hearing aid users were evaluated.
▪The program consisted of 30-minute training sessions by an expert and daily self-HRT.
▪The higher compliance rate suggests that short-time/face-toface HRT is effective.
▪Consonant perception tests and questionnaires scores significantly improved.
CONFLICT OF INTERESTThis study was partially funded by GN ReSound. No other potential conflicts of interest relevant to this article were reported. NotesAUTHOR CONTRIBUTIONS Conceptualization: JMP, SYP, SNP. Data curation: JSH, JMP, YK. Formal analysis: JSH. Funding acquisition: SNP. Methodology: JSH, JMP, YK, SNP. Project administration: JSH, JMP, YK, SNP. Visualization: JSH. Writing–original draft: JSH, SNP. Writing–review & editing: JMP, YK, JHS, DKK, SYP, SNP. ACKNOWLEDGMENTSThis study was partially funded by GN ReSound.
Statistical consultation was supported by the Department of Biostatistics of the Catholic Research Coordinating Center.
Fig. 2.A schematic presentation of the hearing rehabilitation training (HRT) protocol. The HRT program consisted of face-to-face training and self-home training with three interviews with an ENT doctor. A 30-minute face-to-face training was conducted once a week for 8 weeks, with the first 4-week period involving constant discrimination retraining and weeks 5–8 focusing on identification and understanding training. At the same time, patients were taught to perform self-home training every day at home. In the training process, the 10 most commonly used Korean consonants were used for training, starting with low-frequency consonants and gradually progressing to high-frequency consonants. The doctor’s role during our HRT program was to interview the patient three times (HRT prescription, reinforcement, and final motivation for self-HRT). AV, auditory-visua; AO, auditory-only. 
Fig. 3.Baseline results of pure tone audiometry (PTA; A) and word recognition score (B) show no significant differences between the auditory training group and the control group (P>0.05, Mann-Whitney test or t-test). Error bars indicate standard deviation. HRTG, hearing rehabilitation therapy group; CG, control group. 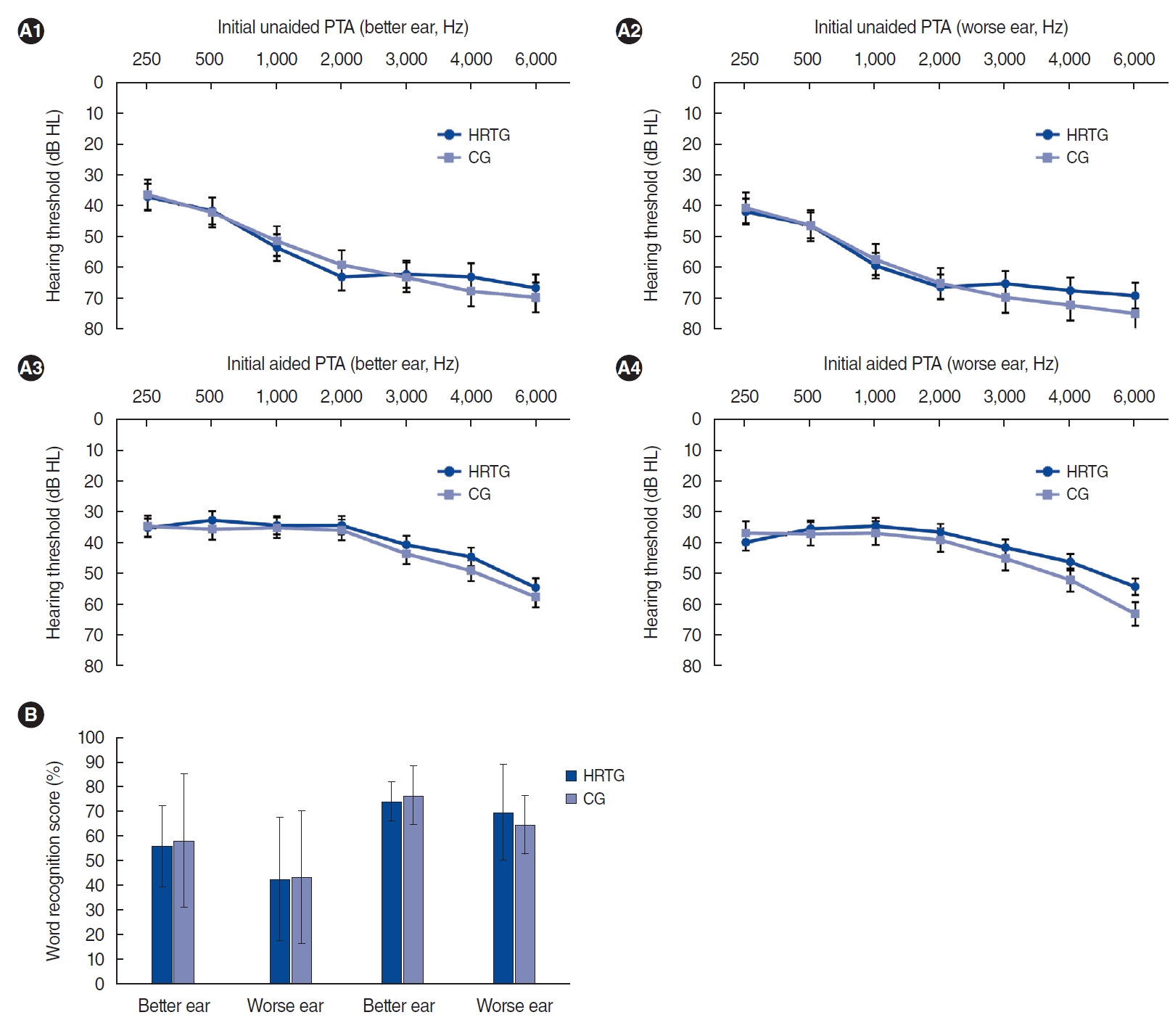
Fig. 4.Changes in scores of the Korean consonant perception tests. Significantly higher mean changes in scores were observed in the HRTG under both consonant-only and consonant+vowel conditions (*P<0.05, Mann-Whitney test). A box and whisker plot shows summary of a set of data: maximum, 75th percentile; median, 25th percentile; and minimum. HRTG, hearing rehabilitation therapy group; CG, control group. 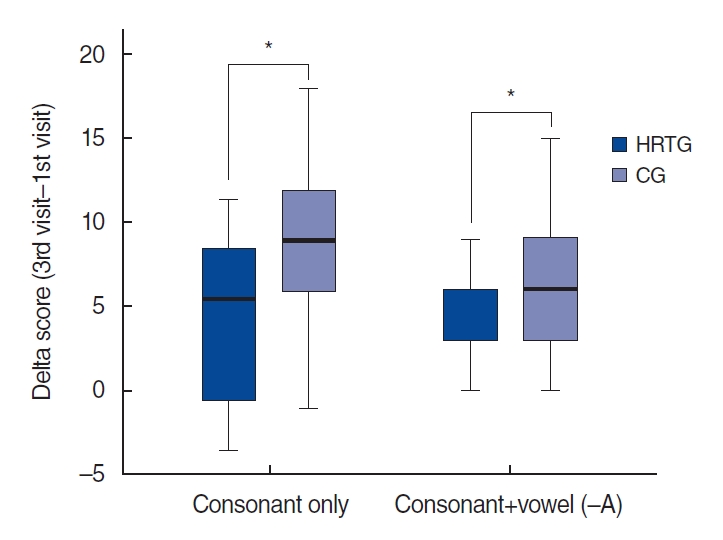
Fig. 5.Changes in hearing questionnaire scores. (A) The Korean version of the International Outcome Inventory for Hearing Aids (K-IOI-HA) score gradually increased in the hearing rehabilitation therapy group (HRTG), but no significant change was observed in the control group (CG), indicating that the HRTG had higher satisfaction than the CG with hearing aid use. Total (B), situational (C), and emotional (D) scores on the Korean version of the Hearing Handicap Inventory (K-HHIE) questionnaire significantly decreased in the HRTG, while no changes were observed in the CG, indicating that the level of discomfort regarding hearing loss significantly decreased after HRT. ***P<0.001, linear mixedeffects model. 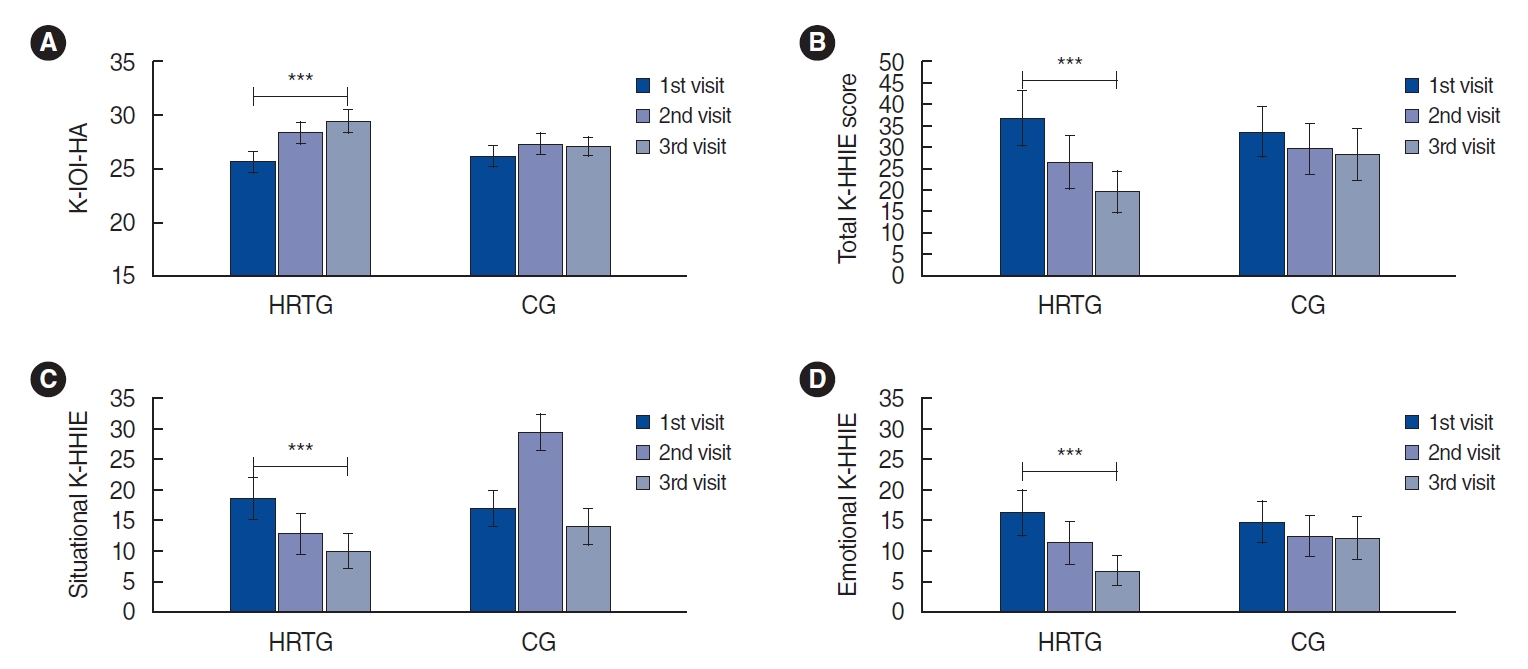
Table 1.Clinical characteristics of the participants
Table 2.Evaluation of the therapeutic effectiveness of the hearing rehabilitation therapy program
Table 3.Summary of randomized controlled trials for auditory training in hearing aid users
HA, hearing aid; WRS, word recognition score; CPT, consonant perception test; SPIN, speech perception in noise; HHIE, Hearing Handicap Inventory for the Elderly; IOI-HA, International Outcome Inventory for Hearing Aids; HHQ, Hearing Handicap Questionnaire; SAC, Self-Assessment of Communication; QDS, Quantified Denver Scale of Communicative Function; Ryff, Ryff Psychological Well-Being Scale; SF-36 PCS, short-form 36 physical component score; COSI, Client Oriented Scale of Improvement; WHODAS II, World Health Organization Disability Assessment Schedule II; CST, Connected Speech Test; CID, Central Institute for the Deaf Sentence Materials; PHAP, Profile of Hearing Aid Performance; HASS, Hearing Aid Satisfaction Survey; ANL, acceptable noise level; NST, Nonsense Syllable Test; LACE, Listening and Communication Enhancement; QuickSIN, Quick Speech In Noise; HINT, Hearing in Noise Test; CSOA, Communication Scale for Older Adults. REFERENCES1. Olusanya BO, Davis AC, Hoffman HJ. Hearing loss: rising prevalence and impact. Bull World Health Organ. 2019 Oct 1; 97(10):646A.
3. Ng JH, Loke AY. Determinants of hearing-aid adoption and use among the elderly: a systematic review. Int J Audiol. 2015 May;54(5):291-300.
4. Chisolm TH, Johnson CE, Danhauer JL, Portz LJ, Abrams HB, Lesner S, et al. A systematic review of health-related quality of life and hearing aids: final report of the American Academy of Audiology Task Force on the Health-Related Quality of Life Benefits of Amplification in Adults. J Am Acad Audiol. 2007 Feb;18(2):151-83.
5. Bisgaard N, Ruf S. Findings from EuroTrak surveys from 2009 to 2015: hearing loss prevalence, hearing aid adoption, and benefits of hearing aid use. Am J Audiol. 2017 Oct;26(3S):451-61.
6. Moon IJ, Baek SY, Cho YS. Hearing aid use and associated factors in South Korea. Medicine (Baltimore). 2015 Oct;94(42):e1580.
7. Kochkin S. MarkeTrak V: “Why my hearing aids are in the drawer”: the consumers’ perspective. Hear J. 2000 Feb;53(2):34-41.
8. Houston DM, Bergeson TR. Hearing versus listening: attention to speech and its role in language acquisition in deaf infants with cochlear implants. Lingua. 2014 Jan;139:10-25.
9. Henshaw H, Ferguson MA. Efficacy of individual computer-based auditory training for people with hearing loss: a systematic review of the evidence. PLoS One. 2013 May;8(5):e62836.
10. Saunders GH, Smith SL, Chisolm TH, Frederick MT, McArdle RA, Wilson RH. A randomized control trial: supplementing hearing aid use with listening and communication enhancement (LACE) auditory training. Ear Hear. 2016 Jul-Aug;37(4):381-96.
11. Sommers MS, Tye-Murray N, Barcroft J, Spehar BP. The effects of meaning-based auditory training on behavioral measures of perceptual effort in individuals with impaired hearing. Semin Hear. 2015 Nov;36(4):263-72.
12. Yu J, Jeon H, Song C, Han W. Speech perception enhancement in elderly hearing aid users using an auditory training program for mobile devices. Geriatr Gerontol Int. 2017 Jan;17(1):61-8.
13. Olusanya BO, Davis AC, Hoffman HJ. Hearing loss grades and the International Classification of Functioning, Disability and Health. Bull World Health Organ. 2019 Oct;97(10):725-8.
14. Song YJ, Lee HJ, Jang HS. A study on the development of KNISEDASP (KNISE-Developmental Assessment of Speech Perception) for auditory training. Asan: Korea National Institute for Special Education; 2010.
15. Kim JS, Shin EY, Shin HW, Lee KD. Development of Korean Consonant Perception Test. J Acoust Soc Korea. 2011 Jul;30(5):295-302.
16. An LJ, Kim JS, Pae SY. The study on developing a test of speech perception in noise. Korean J Audiol. 2002 Dec;6(2):118-27.
17. Chu H, Cho YS, Park SN, Byun JY, Shin JE, Han GC, et al. Standardization for a Korean Adaptation of the International Outcome Inventory for Hearing Aids: study of validity and reliability. Korean J Otorhinolaryngol-Head Neck Surg. 2012 Jan;55(1):20-5.
18. Park SN, Han GC, Cho YS, Byun JY, Shin JE, Chu HS, et al. Standardization for a Korean version of Hearing Handicap Inventory for the elderly. Korean J Otorhinolaryngol-Head Neck Surg. 2011 Dec;54(12):828-34.
19. Weinstein BE. Outcome measures in the hearing aid fitting/selection process. Trends Amplif. 1997 Dec;2(4):117-37.
20. Chisolm TH, Saunders GH, Frederick MT, McArdle RA, Smith SL, Wilson RH. Learning to listen again: the role of compliance in auditory training for adults with hearing loss. Am J Audiol. 2013 Dec;22(2):339-42.
21. Hickson L, Worrall L, Scarinci N. A randomized controlled trial evaluating the active communication education program for older people with hearing impairment. Ear Hear. 2007 Apr;28(2):212-30.
22. Preminger JE, Ziegler CH. Can auditory and visual speech perception be trained within a group setting. Am J Audiol. 2008 Jun;17(1):80-97.
23. Humes LE, Skinner KG, Kinney DL, Rogers SE, Main AK, Quigley TM. Clinical effectiveness of an at-home auditory training program: a randomized controlled trial. Ear Hear. 2019 Sep/Oct;40(5):1043-60.
24. Sweetow RW, Sabes JH. The need for and development of an adaptive Listening and Communication Enhancement (LACE) Program. J Am Acad Audiol. 2006 Sep;17(8):538-58.
25. Stecker GC, Bowman GA, Yund EW, Herron TJ, Roup CM, Woods DL. Perceptual training improves syllable identification in new and experienced hearing aid users. J Rehabil Res Dev. 2006 Jul-Aug;43(4):537-52.
26. Molloy K, Moore DR, Sohoglu E, Amitay S. Less is more: latent learning is maximized by shorter training sessions in auditory perceptual learning. PLoS One. 2012;7(5):e36929.
27. Boothroyd A. Adult aural rehabilitation: what is it and does it work. Trends Amplif. 2007 Jun;11(2):63-71.
28. de Miranda EC, Gil D, Iorio MC. Formal auditory training in elderly hearing aid users. Braz J Otorhinolaryngol. 2008 Nov-Dec;74(6):919-25.
29. Lundberg M, Andersson G, Lunner T. A randomized, controlled trial of the short-term effects of complementing an educational program for hearing aid users with telephone consultations. J Am Acad Audiol. 2011 Nov-Dec;22(10):654-62.
|
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||