Decreased Serum Epinephrine in Children With Positive Skin Prick Test
Article information
Abstract
Objectives
To evaluate the association between catecholamine levels and skin prick test results among children.
Methods
Two hundred eight first grade children from one elementary school were invited to participate in this study. Skin prick test (SPT) for six allergens (2 house dust mites, cat, dog, mugwort, and pollen mixture) was performed, and patient demographic information was recorded. The parents were surveyed using questionnaires about rhinitis-related symptoms. Finally, venous blood sampling was done to measure catecholamine levels (epinephrine, norepinephrine, and dopamine) by high-performance liquid chromatography.
Results
Out of 208 children, 174 (106 boys and 68 girls) enrolled in this study. Ninety-six of the children (55%) had negative SPT (nonsensitization group), while 78 (45%) had a positive SPT to at least one of six allergens (sensitization group). The diagnosis of chronic rhinitis was more prevalent in the sensitization group (35.9%) than nonsensitization group (26.0%), however the finding was not significant (P=0.186). Epinephrine levels were decreased between the sensitization group compared to the nonsensitization group (P=0.004). There was no difference in norepinephrine and dopamine levels (P>0.05).
Conclusion
Epinephrine levels are lower in children with positive SPT compared to controls, however, the level of the catecholamine was not associated with the presence or absence of rhinitis symptoms.
INTRODUCTION
Epinephrine is an α- and β-adrenergic agonist that promotes vasoconstriction and bronchodilation, increases blood pressure, chronotropy and inotropy, while decreasing capillary leakage [123]. Epinephrine is a catecholamine that is primarily produced by the adrenal gland and the postganglionic fibers of the sympathetic nervous system [1]. The most abundant catecholamines are epinephrine, norepinephrine, and dopamine [4]. Dopamine converts serially to norepinephrine then to epinephrine [4]. A small amount of these catecholamines are present in the blood, mostly through spillover from the synapses of the sympathetic system [45].
Allergic symptoms vary depending on host, environmental factors, and involved organ system [678]. For example, nasal congestion and rhinorrhea are the most common symptoms in allergic rhinitis [6], wheezing and shortness of breath in asthma [8], and a sudden decrease in blood pressure and dyspnea in anaphylactic shock [7]. Despite a wide variety of symptoms, allergic diseases demonstrate similarities in pathophysiology including vasodilatation, capillary leakage, bronchoconstriction, etc. [678]. Until recently, the pathophysiology of allergy has been largely considered to be a result of an overreaction to histamine and other allergic mediators. However, from a different perspective, these allergic findings might also be dependent on levels of epinephrine. Our hypothesis was that decreased epinephrine or other catecholamines might contribute to allergy or skin prick test (SPT) results. The blood levels of epinephrine and other catecholamines in allergic patients have not been studied thoroughly.
The purpose of this study was to evaluate the blood levels of epinephrine and other catecholamines in allergic and control patients.
MATERIALS AND METHODS
Subjects and methods
Two hundred eight children in the first grade from a public elementary school in Seoul, South Korea were invited to participate in this study. This study was approved by Konkuk University Hospital Institutional Review Board (KUH1110015) and registered in Clinical Research Information Service (KCT0000699). Written informed consent was acquired from the children's parents prior to enrolling in the study.
No medication use was permitted 2 weeks prior to enrollment or during the study. Body mass index, age, sex, and presence of absence of chronic rhinitis was evaluated and recorded. A SPT and blood sampling were completed between 9:00 AM to 11:00 AM under fasting conditions to reduce diurnal and other variations [145].
SPT was done for six most common allergens for Korean children, namely Dermatophagoides pteronyssinus, Dermatophagoides farinae, cat, dog, mugwort, and pollen mixture [9]. If the wheal was larger than 3 mm with a positive histamine control, it was defined to be a positive SPT. The parents or guardian were surveyed using questionnaires about rhinitis-related symptoms. Chronic rhinitis was defined if children had more than two symptoms out of the five (nasal obstruction, runny nose, sneezing, and itchy eye or nose) for more than 3 months. Venous blood sampling was collected at the antecubital vein. Catecholamine (epinephrine, norepinephrine, and dopamine) levels were measured using a high-performance liquid chromatography. Briefly, the blood was collected into ethylenediaminetetraacetic acid (EDTA) tubes and the plasma was separated by centrifugation. One milliliter of plasma was mixed with 30 mg of alumina, 200 µL of dihydroxybenzylamine, and 1 mL of Tris buffer, then centrifuged. After discarding supernatant, 150 µL of the 0.1 M phosphoric acid was added. After centrifugation, the supernatant was injected onto the column. Electrochemical detection of the catecholamines was achieved using a Coulochem III Electrochemical Detector (ThermoScientific, Sunnyvale, CA, USA) fitted with a guard cell and an analytical cell. Oxidation of the analytes was set potentials 1 (-300 mV, sensitivity at 10 µA) and set potential 2 (450 mV, sensitivity set at 50 nA). The mobile phase consisted of diammonium hydrogen orthophosphate containing heptane sulphonic acid and EDTA adjusted to pH 3.5. Agilent Poroshell 2.7-µm analytical column (Agilent Technologies, Berkshire, UK) was used at a flow rate of 1.0 mL/min.
Statistics
Catecholamine levels and the other data were compared between children with positive SPT for at least one of six allergens (sensitization group) and those with negative SPT for all six allergens (nonsensitization group). The comparison of catecholamine level and body mass index was carried out by using a Student t-test, and those of sex ratio and prevalence of chronic rhinitis was done by using chi-square test. The P-value were reported 2-sided where the statistical significance was set at <0.05. These calculations were completed with IBM SPSS ver. 20.0 (IBM Co., Armonk, NY, USA).
RESULTS
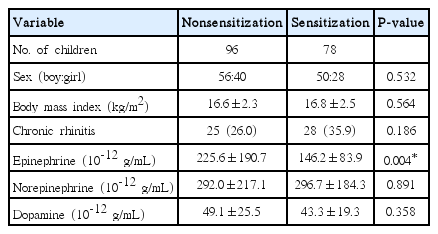
Of the 208 children, 174 (106 boys and 68 girls) enrolled in the study and met eligibility requirements (Table 1). The mean age of the children in the study was 7 years old (range, 6.5 to 7.5 years). Among them, 96 did not show any positive allergens (nonsensitization group), while 78 had a positive SPT for at least one of six allergens (sensitization group). The most common allergens were D. pteronyssinus and D. farina. The positive rates for them were 27.4% and 36.5%, respectively. Other allergen rates were 4.3% for cat, 6.7% for dog, 1.4% for mugwort, and 1.4% for pollen mixture. Sixty-four children out of 78 (82.1%) had positive SPT to one or two allergens, while 14 children (17.9%) had three or more positive allergens.
Sex and body mass index were not different between sensitization and nonsensitization groups (P=0.532 and P=0.564, respectively). The prevalence of chronic rhinitis was higher in the sensitization group (35.9%) than the nonsensitization group (26.0%), however these results did not reach statistical significance (P=0.186).
Epinephrine levels in the nonsensitization group were significantly higher than from children in the sensitization group (P=0.004). However, there was no difference in norepinephrine and dopamine levels between the two groups (P=0.891 and P=0.358, respectively).
DISCUSSION
Among the diverse mechanisms of allergic rhinitis, a dysregulation of autonomic nerves has been suspected [6]. In fact, surgical excision of the autonomic nerves in the nasal cavity has shown some effectiveness in reducing allergic rhinitis symptoms, probably due to decreased parasympathetic stimulation [10]. Furthermore, epinephrine and other sympathomimetics are used for the treatment of a variety of allergic diseases [11]. For example, an injection of epinephrine is the first-line treatment for an anaphylactic shock [7]. Sympathomimetics including oxymetazoline nasal spray and pseudoephedrine are commonly used medications for allergic rhinitis [6]. Sambutol is another sympathomimetic used as bronchodilator for an allergic asthma [8]. Therefore, we can infer an association between allergic disease and a variety of neurotransmitters from the autonomic nervous system.
In this study, epinephrine levels were decreased in children with a positive SPT compared to those with a negative SPT, as we hypothesized. It is possible that capillary leakage and vasodilation might occur more easily in patients with decreased serum epinephrine, which could also aggravate skin swelling and redness during SPT.
We also presumed that decreased serum epinephrine levels could contribute to an increase in allergic symptoms. Clinically, a positive SPT does not always equate to symptomatic disease. Only when a positive SPT accompanies clinical symptoms, do we diagnose an "allergic disease" such as allergic rhinitis, allergic asthma, or allergic conjunctivitis. When a SPT is positive without coexisting symptoms, it is considered to be a subclinical allergy. In this study, out of the 78 children with positive SPT, only 28 had chronic rhinitis symptoms. Therefore only 28 patients are considered to have allergic rhinitis. The remaining 50 children with a positive SPT without symptoms have subclinical allergy. To date, there is no accepted explanation why patients with positive SPT have either allergy or subclinical allergy. We hypnotized that a positive SPT would first occur when epinephrine levels decreased to a certain threshold, at which clinical symptoms might not yet develop (subclinical allergy status). In this theory, only when epinephrine levels further decrease would symptoms develop (allergic rhinitis status). However, in this study, there was no difference in epinephrine levels between children with allergic rhinitis (160.3±59.1×10-12 g/mL) and subclinical allergies (139.3±93.4×10-12 g/mL, P=0.338) on high-performance liquid chromatography. One possible explanation of this finding is that lower level of serum epinephrine might not be not solely responsible for rhinitis symptoms, and that the development of allergic rhinitis is multifactorial.
Konno et al. [12] evaluated the relationship between serum catecholamine levels and nasal patency. The authors found that psychic stimulation increased plasma levels of norepinephrine and epinephrine in 6 minutes in allergic patients and controls, which improved nasal patency in both groups. These results agree with our initial hypothesis that increased blood catecholamine levels correlate with decreased rhinitis symptoms such as nasal obstruction.
There are several limitations for our study. First, catecholamines are well-known to show diurnal variation. However, we measured it only once due to the limited resources. Second, the patients were only asked about rhinitis-related symptoms, so the association of catecholamine levels with other allergic diseases such as atopic dermatitis or allergic asthma was not evaluated. Next, we did not measure epinephrine levels directly from nasal mucosa. If this were done, we could provide stronger evidence about a potential association between changes in epinephrine levels and allergic symptoms. In addition, we have no explanation why dopamine and norepinephrine levels were not different between sensitization and nonsensitization group. It is possible the current study is underpowered to detect differences in these catecholamines between the groups.
In conclusion, serum levels of epinephrine are decreased among children with a positive SPT compared to controls. However, this level was not associated with the presence or absence of the rhinitis symptoms.
ACKNOWLEDGMENTS
This research was supported by Konkuk University in 2012 (grant number: 2012-A019-0327).
Notes
CONFLICT OF INTEREST: No potential conflict of interest relevant to this article was reported.